Total Hip Replacement
What is a Total Hip Replacement?
A Total Hip Replacement (THR) is where a damaged hip joint is replaced with prosthetic components in the aim of improving movement, decreasing pain and providing better function and quality of life.
JL PhysioFit
Anatomy of the Hip Joint?
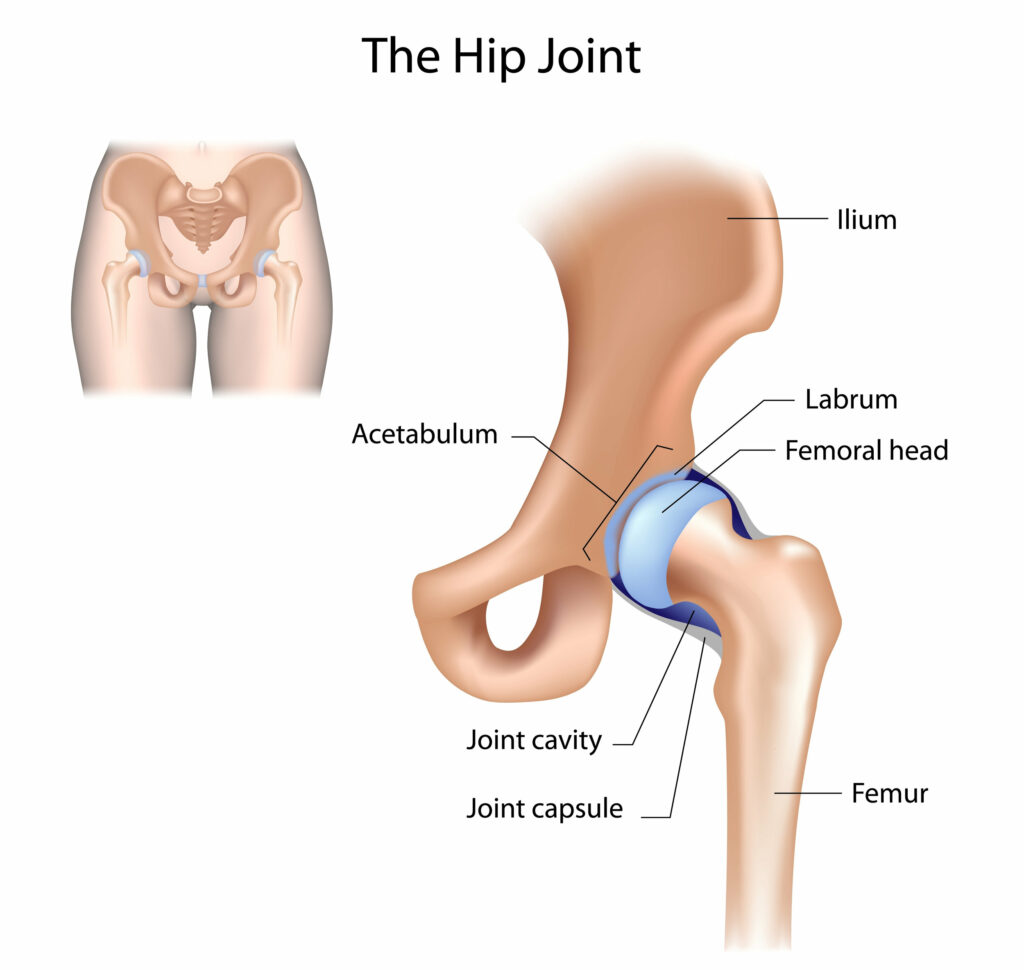
The hip joint is one of the largest joints in the body and is classed as a ball-and-socket joint. It is comprised of the articulation between the top of the femur (thigh bone), which is the ball, and the acetabulum of the pelvis (socket). The ends of these bones are covered with smooth articular cartilage, a substance that protects the bone and also aids movement.
Between the joint space lies the labrum, which is a ring like structure that provides smooth movement and shock absorption. Surrounding the whole joint is the joint capsule, it is through this structure that the joint is nourished with synovial fluid (WD-40).
Then we have a number of strong ligaments that attach in and around the hip joint to provide stability. A ligament attaches bone to bone. Similarly, we have various muscles that attach in and around the hip joint that allows us to move the hip.
Who needs a THR?
The vast majority of people that end up having a THR are those in which arthritis has damaged the joint severely. It is also common in elderly people and those that have fallen and fractured their hip. Other conditions like childhood hip disease, rheumatoid arthritis, osteonecrosis and post traumatic arthritis are common causes that can make you a candidate for surgery.
The decision to have THR surgery should be one which is considered carefully and in consultation with medical professionals like your doctor, physiotherapist and consultant.
Avenues like physiotherapy are very important to try as a first measure as they are non-invasive, very effective and help to strengthen your hip, which is critical to both pre and post op rehabilitation outcomes.
Generally, if you are needing a THR you will have pain when walking or sitting for long periods, and first thing when you wake that can last for hours. You will most likely struggle with daily activities like housework and getting in and out of the car, and your general quality of life will be suffering. Medications for pain relief and anti inflammatories will not have a great effect anymore.
An x-ray is the gold standard for determining the severity of arthritis in the hip joint and is classed as mild, moderate or severe. It must be stressed however, that even if an x-ray deems to show severe OA, this might not correlate to the patient experiencing the same level of pain/discomfort. It is very important to take into consideration your goals and motivations for having a THR, and this would be discussed with your physiotherapist.
How is it done?
Each surgeon may have different or preferred methods so it is important to ask about this prior to your operation. Below is an example of how a typical THR is done:
- The damaged ball of the femur (thigh bone) is removed and replaced with a metal stem that goes down the middle of the bone.
- The surgeon then replaces the head of the femur (ball of the joint) with a metal or ceramic ball.
- Then the original damaged socket (acetabulum) will then be replaced with a metal one.
- A plastic, metal or ceramic spacer is then fitted between the new ball and the socket, before the ball is fixed in place. This helps with mobility and stability of your new hip joint and acts as your new labrum (cartilage).
Pre and post operation Physiotherapy at JL Physiofit?
We work with clients both pre and post-surgery. This allows a number of benefits:
JL PhysioFit
Pre surgery:
Following an initial detailed assessment, we will be better placed to form a plan that suits your needs and works around your life.
We provide all of our clients with a ‘THR Surgery Booklet’, so they are more prepared for surgery, what it entails and the likely aftercare they need, and what milestones they should be aiming for.
Clients are able to maintain and strengthen the muscles around the hip joint so that it makes recovery more manageable and aids better outcomes.
Forming a team between patient and physio helps to provide a lot of support both physically and mentally for what can be a stressful period of life.
Some patients may improve to the point where they delay their operation.
JL PhysioFit
Post-Surgery:
Assessment of the hip, how it is moving and feeling along with gentle exercises to begin with.
Clear plan in place to start rehabilitation of the hip and working towards key milestones.
Our ‘THR Surgery Booklet’ will be given to patients and this will help them to understand more about what to do and what not to do as they progress from the early stages of recovery, right through to end stage rehab.
We have the facilities to guide patients through the whole process to ensure best possible outcomes for them.
How long will we work together and what will it look like?
Pre operatively, we will most likely work together for 3-6 months (largely dependent on when your operation is) to ensure we have the best chance of strengthening the hip as much as we can before the operation.
Post operatively, we work with clients a minimum of 3 months but usually beyond this as well. This gives us time to make sure we are on the right track and you are progressing as you should be.
Often in the first few weeks we will be helping you regain movement and ease pain using various hands-on techniques, whilst also building exercises in a manageable way. You will be very clear on what you need to do outside of the sessions.
As the weeks progress, we will develop your exercise programme as well as work with you 1:1 in the rehab room and carry out exercise sessions together.
Once the initial 3 months are up, clients are a lot more confident with their hip and what needs to be done to continue the good work. At this stage we have a conversation about how to manage things going forward.
Often clients end up working with us longer as they want to continue to strengthen under the guidance of a physio. Some clients choose to join one of the Physio Led Pilates classes that we teach here, to continue strengthening and get the most out of their new hip.
How do I get started?
The first step is to book an initial Physiotherapy assessment/first appointment. This will allow us to determine the most appropriate pathway for your situation.
If you are ready to book in then you can either phone the main desk on 0191 814 9717, or use our easy online booking system by clicking here and selecting the ‘Physiotherapy Assessment/First Appointment’ option at a day and time that suits you. You will usually be offered an appointment within 48 hours.
Like to speak to someone first?
No problem, please call the main desk and if needed we can have a physio call you back to discuss your specific situation.
Testimonials
What Our Clients Say





